A familiar story plays out in a lot of diets. The scale drops, routines tighten up, and then months later the weight creeps back.
A new long-term study suggests that this “yo-yo” pattern can still leave a lasting imprint on health, even when the pounds return.
The work tracked people enrolled in two structured weight-loss trials years apart. Many who returned for a second round started that second program at nearly the same body size as before. Yet their internal fat pattern and blood markers looked better than they did at the very start.
“Yo-yo dieting” usually describes repeated cycles of intentional weight loss and gradual regain. The concern is that those cycles might harm health, not just morale. This study focused on a specific issue: visceral fat, the metabolically active fat stored deep in the abdomen around internal organs. High levels are linked to cardiometabolic disease.

Prof. Iris Shai, the study’s principal investigator from Ben-Gurion University of the Negev, dean of the School of Sustainability at Reichman University, an adjunct professor at Harvard T.H. Chan School of Public Health, and an honorary professor at Leipzig University, Germany, framed the results as a challenge to the “numbers game” approach to weight.
“Persistent commitment to a healthy dietary change creates cardiometabolic memory in the body,” Shai said. She added that repeated participation in a structured lifestyle program, even after an apparent “failure,” “may lead to significant and sustainable health benefits over the years, particularly through the reduction of harmful visceral (abdominal) fat.”
Hadar Klein, RD MSc, the lead author and a doctoral student, argued that judging success by weight alone misses the point. “Body weight alone does not capture changes in visceral fat or metabolic biomarkers,” Klein said. “Even when weight is regained, cardiometabolic health may remain improved, and success should not be defined solely by the number on the scale. Importantly, even when weight loss is attenuated during a second attempt, the cumulative benefits for abdominal fat and metabolic health are substantial”.
The study, published in BMC Medicine, followed participants from two consecutive 18-month randomized controlled dietary trials: CENTRAL (conducted 2012–2014) and DIRECT-PLUS (conducted 2017–2018). Together, the trials enrolled 480 people, and the analysis included 572 trial observations.
Both trials took place at the same workplace research site in Dimona, in southern Israel. Each trial used Mediterranean diet based approaches and physical activity components, compared with control diets. Researchers also used detailed MRI scans before and after each intervention to measure abdominal fat compartments.
One key subgroup mattered most for the “yo-yo” question: 92 participants took part in both trials, called “rejoiners.” At long-term follow-up, 384 of the 480 participants, or 80%, returned for MRI and clinical assessments conducted during 2022–2024. Among the rejoiners, 76 of 92, or 83%, were re-evaluated.
Most participants were men. At follow-up, the mean age was 57.1 years, and 89% were male.
During the first trial, people who later rejoined the second trial responded much like those who only did the first trial once. Weight loss during that initial intervention looked nearly identical: -3.4% for future rejoiners versus -3.3% for those who did not return.
Then time passed, and many regained weight.
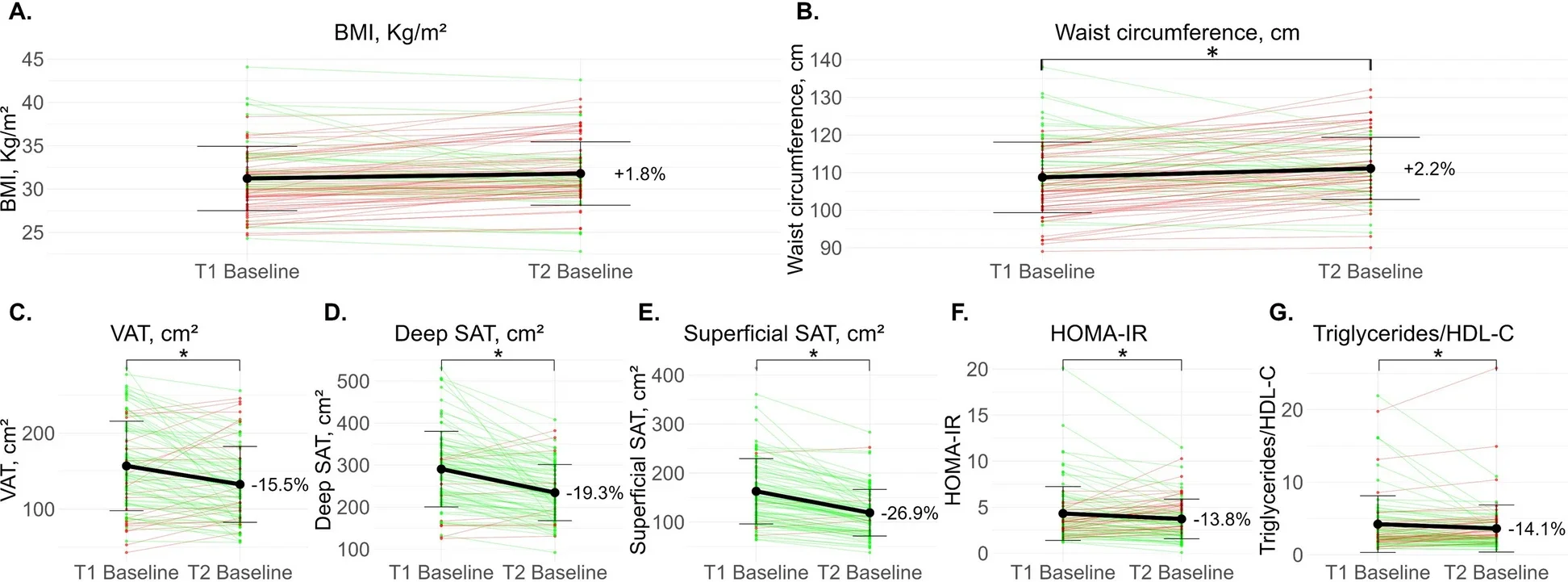
When the rejoiners started the second trial, their baseline body size looked much like it had at the start of the first. Their average body mass index was 31.8 kg/m² at the start of the second intervention, compared with 31.3 kg/m² at the start of the first.
The surprise was inside the abdomen.
At the start of the second trial, those rejoiners had less visceral adipose tissue than they did at their very first baseline: 135.5 cm² versus 160.0 cm². They also had better metabolic measures. Their insulin resistance index, HOMA-IR, was 3.8 compared with 4.5 at the first baseline. Their triglycerides-to-HDL cholesterol ratio was 3.6 compared with 4.2.
Those differences were statistically significant in the study’s analysis.
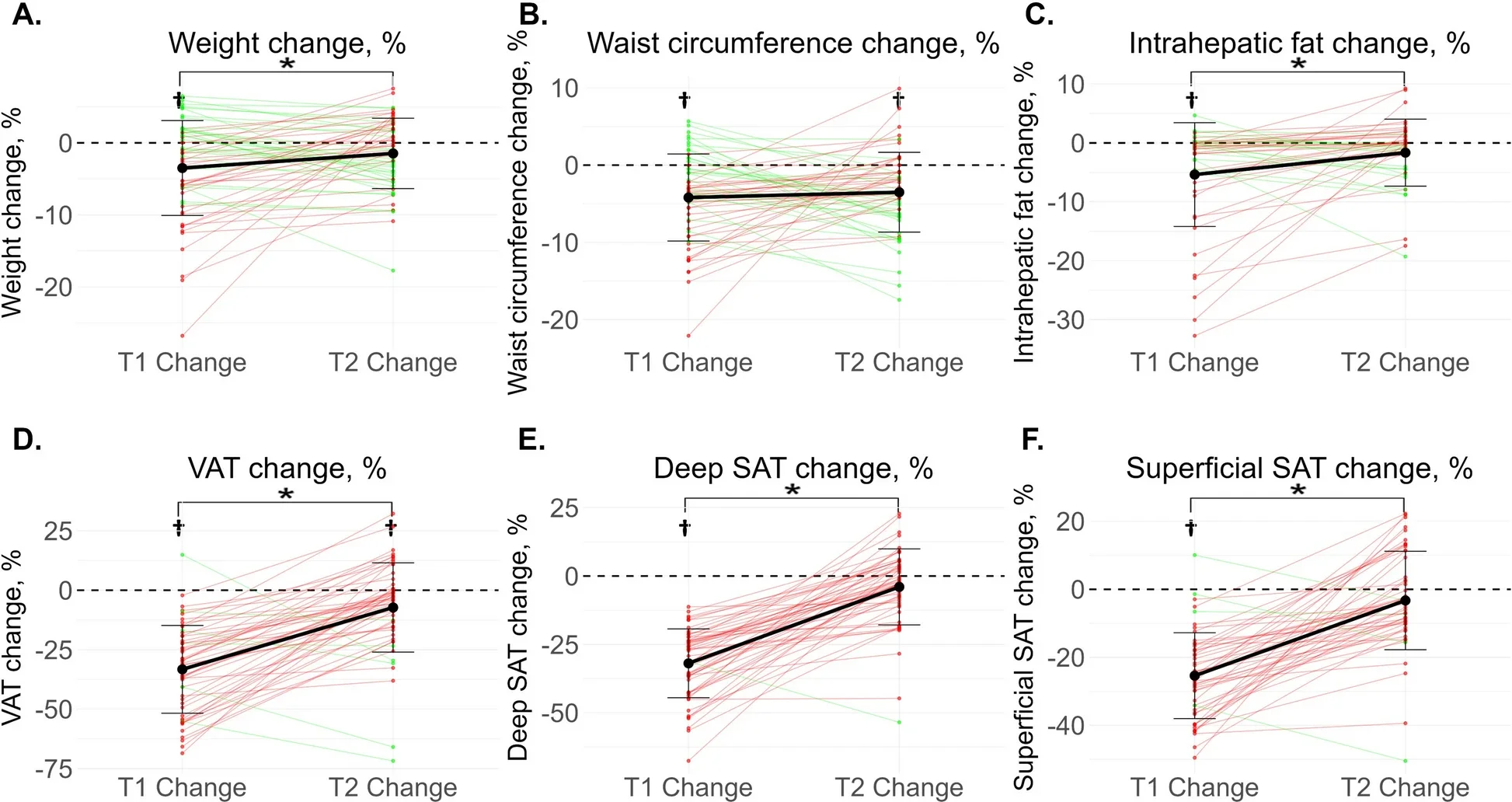
During the second intervention, rejoiners improved again, but not as sharply as they had the first time. Weight fell by -1.5% during the second program, compared with -3.5% during the first. Visceral fat fell by -7.2% during the second, compared with -33.3% during the first.
Deep subcutaneous fat and superficial subcutaneous fat also dropped less during the second intervention than during the first.
That muted response was not explained, in this dataset, by obvious gaps in effort. The study reports that reductions in daily energy intake and increases in physical activity did not differ significantly between rejoiners and single-time participants in either trial.
One sentence kept coming up in the results: you can lose less this time and still be better off later.
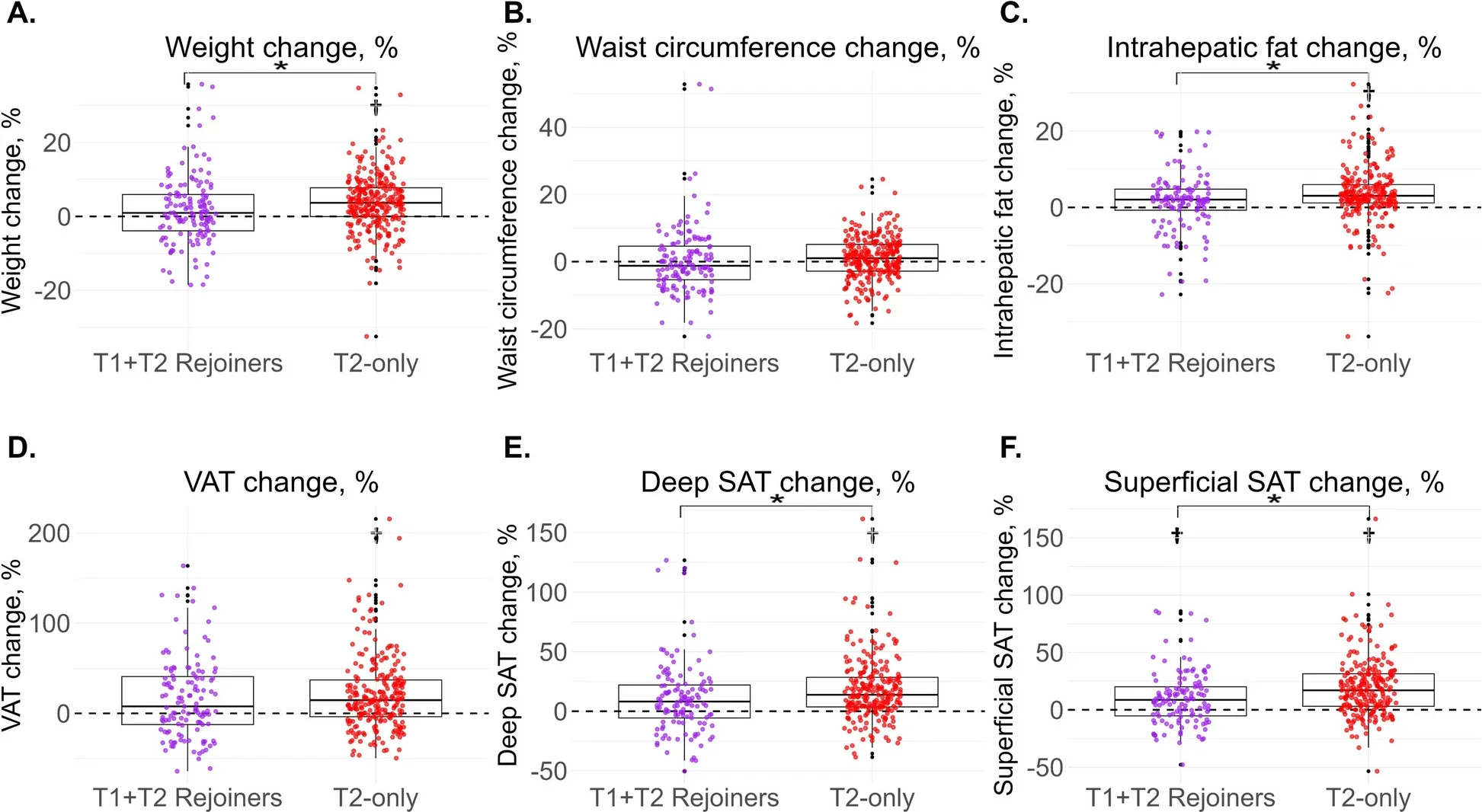
Five years after the second trial ended, rejoiners had less weight regain than people who only participated in the second trial once. Rejoiners averaged +0.2% weight regain, compared with +2.9% among first-time second-trial participants. They also had less regain of deep subcutaneous fat (+2.4% versus +13.3%) and superficial subcutaneous fat (+12.8% versus +24.3%). Visceral fat regain was similar between those groups.
Across the broader follow-up picture, many metabolic benefits faded by the 10-year mark among people who only participated in the first trial. The rejoiners, by contrast, maintained stability in several measures over that same period, including waist circumference and some metabolic indices listed in the paper.
The rejoiner group was modest in size, even though it was followed intensively across five time points. The authors also note limits on generalizability: rejoiners were self-selected, and the cohort was predominantly male, reflecting the workplace setting.
Still, the study’s strength is its repeated MRI imaging and long-term tracking, using consistent protocols across the original interventions and the follow-up period.
Research findings are available online in the journal BMC Medicine.
The original story “Researchers reveal the hidden benefits of ‘yo-yo dieting’” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post Researchers reveal the hidden benefits of ‘yo-yo dieting’ appeared first on The Brighter Side of News.