A scoop of fiber stirred into yogurt may not sound like much of a pain treatment. But in a new clinical trial, that simple routine eased knee osteoarthritis pain, improved grip strength, and appeared easier for people to stick with than a digital physiotherapy program.
The study, called INSPIRE, tested inulin, a prebiotic fiber found in foods such as chicory root and Jerusalem artichoke, in adults with knee osteoarthritis. Researchers from the University of Nottingham reported that after six weeks, people taking inulin had less knee pain than those given a placebo. The work was published in Nutrients.
Knee osteoarthritis is one of the most common joint disorders in older adults. It wears down the joint, causing pain, stiffness, and trouble moving around. Exercise is a standard first-line treatment, but many people find it hard to maintain. Pain medicines can help, though they also come with risks.
“This study raises the exciting possibility that a simple dietary change, adding a fibre supplement to your breakfast or yogurt, could meaningfully reduce pain and improve physical function,” said Dr. Afroditi Kouraki of the University of Nottingham’s School of Medicine, the study’s lead author.
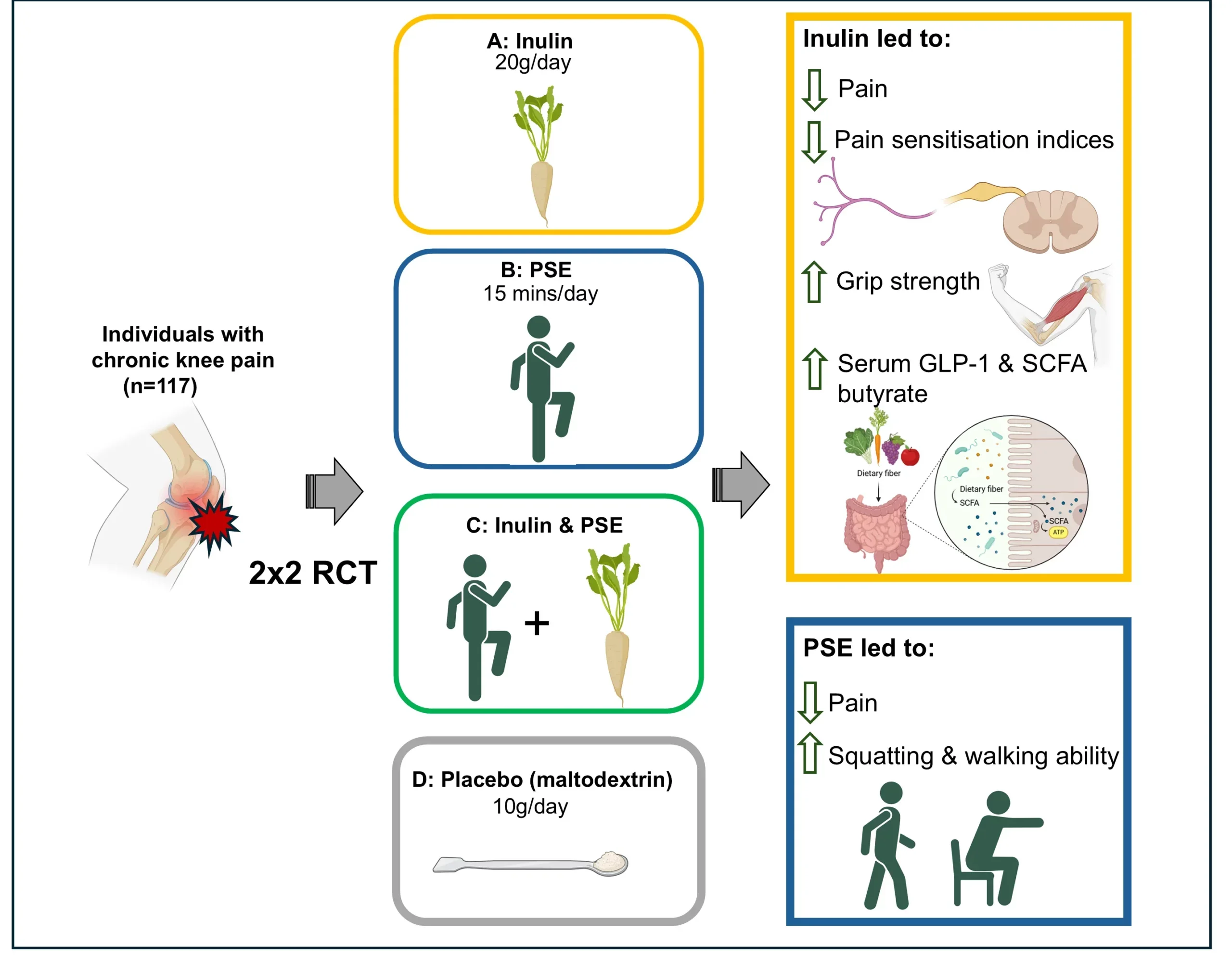
The six-week randomized controlled trial enrolled adults with knee osteoarthritis living in the community around Nottingham. Of 721 people screened, 136 were randomized and 117 completed both baseline and follow-up assessments. The average age was 67.5, the average body mass index was 29.5, and 58.12% of participants were female.
Researchers split participants into four groups: inulin alone, digital physiotherapy-supported exercise alone, both treatments together, or a placebo with usual care. The physiotherapy program was delivered online through the Joint Academy platform. People in the inulin group took 20 grams a day, usually mixed into cereal, smoothies, yogurt, or drinks. The placebo group received 10 grams a day of maltodextrin.
Both inulin and physiotherapy reduced pain compared with placebo. Inulin lowered pain scores by 1.11 points on a 0-to-10 scale, while physiotherapy lowered them by 1.55 points. The combined treatment reduced pain by 1.67 points. All three exceeded the study’s minimum clinically important difference of 1 point.
But the treatments did not work in the same way. Physiotherapy improved squatting ability and walking ability. Inulin did not. Instead, inulin improved grip strength, with a 4.62-point advantage over placebo, while physiotherapy did not improve that measure.
The inulin group also stood out on tests tied to pain sensitivity. Participants taking the fiber supplement were more likely to improve on pressure pain thresholds near the knee and on temporal summation, a measure linked to how the spinal cord processes repeated pain signals. The physiotherapy group did not show those changes.
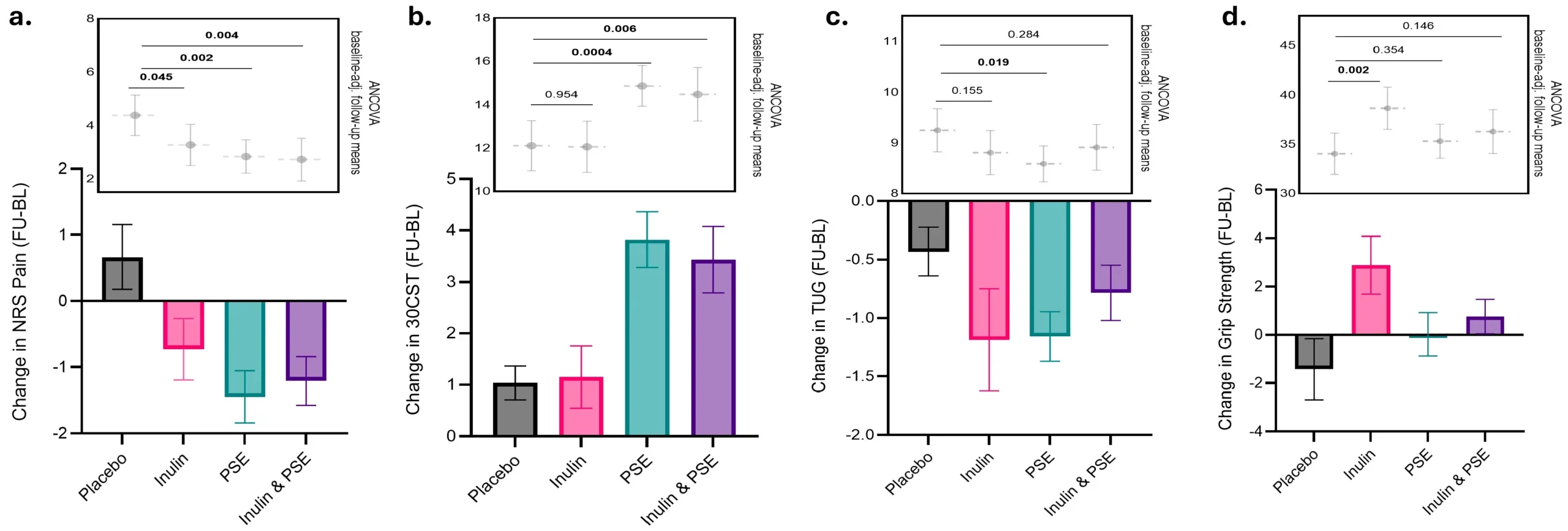
That matters because osteoarthritis pain is not only about damaged joints. The nervous system can also become more sensitive, amplifying discomfort. The authors said the inulin findings suggest that changing the gut environment may influence those pain pathways.
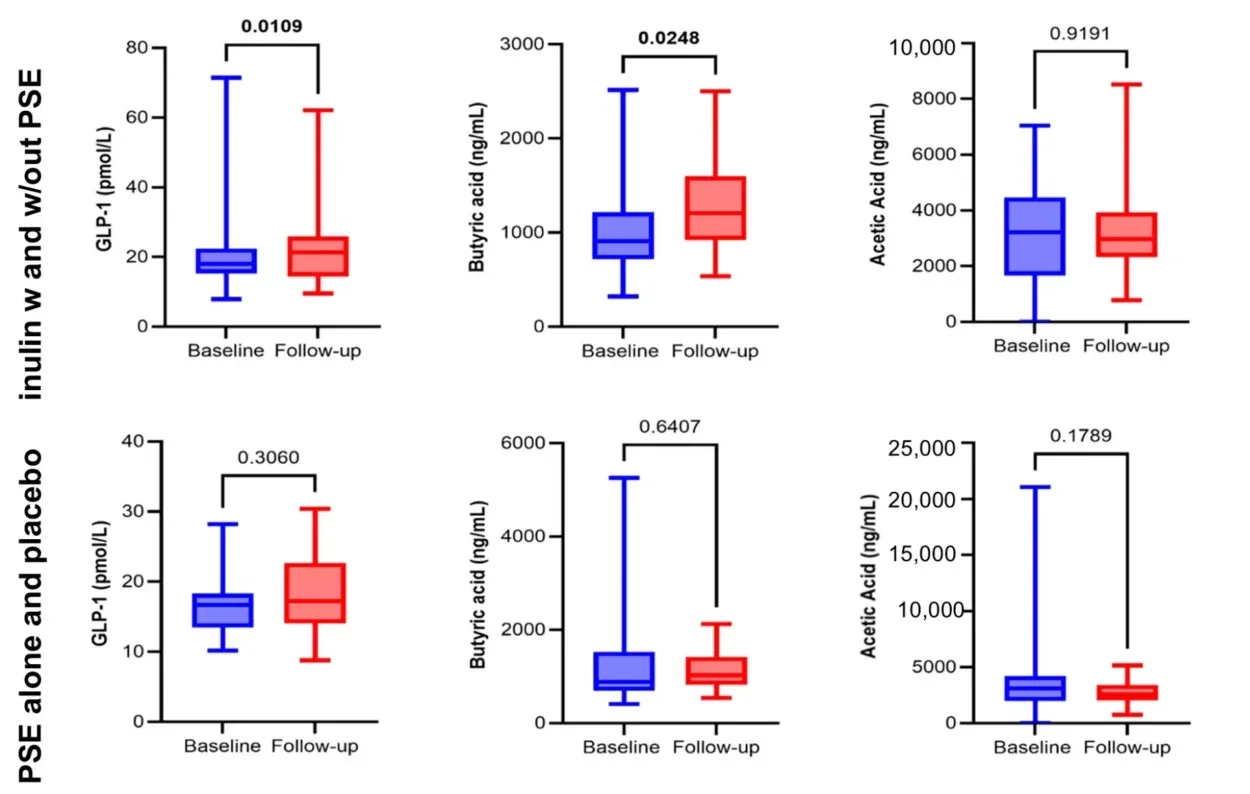
The researchers looked for clues in the blood. Inulin increased butyric acid, a short-chain fatty acid made when gut microbes break down fiber. It also increased glucagon-like peptide-1, or GLP-1, a gut hormone that has been linked to pain regulation and muscle health. Higher GLP-1 levels were associated with stronger grip strength and better self-reported knee function.
Senior author Professor Ana Valdes said that link “is particularly intriguing and points to a broader gut-muscle-pain axis that warrants further investigation.”
One of the sharpest contrasts in the trial was dropout. Just 3.6% of participants in the non-physiotherapy arms withdrew, compared with 21% in the physiotherapy arms. The difference was statistically significant.
That does not mean exercise failed. In fact, it helped pain, walking, and squatting. Still, the gap suggests that a daily supplement may fit more easily into some people’s routines than a program requiring regular guided exercise.
Adherence among those who stayed in the study was high in both groups, averaging 84% for physiotherapy and 88% for inulin. Among 50 participants who completed the inulin intervention, 23 reported minor gastrointestinal side effects such as bloating and wind, but these did not lead to withdrawal or non-compliance. No adverse events were reported in the other groups.
Professor Lucy Donaldson, Director of Research at Arthritis UK, called the work “exciting preliminary research” and said it highlights how diet and physiotherapy may help people with arthritis in different ways.
The study also had limits. Participants could not be blinded to whether they were doing physiotherapy, which may have influenced self-reported pain. The trial lasted only six weeks. Dropout in the exercise arms forced researchers to adjust recruitment later in the study, which weakens the strength of causal inference compared with a fully balanced design. The GLP-1 analysis was exploratory and not part of the original plan, so those findings need independent confirmation. The study was also underpowered to detect whether combining inulin with physiotherapy produced a true synergistic effect.
For now, the study suggests that a prebiotic fiber supplement may offer a low-burden, well-tolerated way to reduce knee osteoarthritis pain, especially for people who struggle to keep up with exercise programs.
It does not replace physiotherapy, which still improved walking and squatting, but it may point toward a broader approach in which diet and movement help different parts of the pain problem.
Research findings are available online in the journal Nutrients.
The original story “Daily fiber supplement relieves arthritis pain, study finds” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post Daily fiber supplement relieves arthritis pain, study finds appeared first on The Brighter Side of News.