A child can struggle for years before anyone puts a name to it.
That is one reason attention-deficit/hyperactivity disorder remains so hard to catch early. Even though the condition affects millions of children, early support can change a great deal. In a new study from Duke Health, researchers found that artificial intelligence can sift through routine electronic health records. It can estimate a child’s risk of developing ADHD years before a typical diagnosis.
The study, published in Nature Mental Health, points to something simple at the center of the work. The clues may already sit inside ordinary medical records created during regular care.
“We have this incredibly rich source of information sitting in electronic health records,” said Elliot Hill, lead author of the study and a data scientist in the Department of Biostatistics & Bioinformatics at Duke University School of Medicine. “The idea was to see whether patterns hidden in that data could help us predict which children might later be diagnosed with ADHD, well before that diagnosis usually happens.”

The researchers said their approach could help primary care providers identify children who may need closer follow-up. It could also help prompt referral for a formal ADHD assessment earlier than they otherwise would.
To build the tool, the Duke team trained a specialized AI model on electronic health records. The broader research involved pretraining an electronic health record foundation model using records from more than 720,000 patients. Then, the team fine-tuned that model to predict the likelihood and timing of ADHD diagnosis from birth to age 9 in a pediatric cohort of more than 140,000 children.
Those records included children with and without ADHD.
The model learned to spot combinations of developmental, behavioral, and clinical events that often appeared years before a diagnosis was made. Instead of relying on one obvious sign, it searched for patterns across the medical history a child built from birth through early childhood.
By age 5, the model reached a time-dependent area under the receiver operating characteristic curve of 0.92 at a four-year time horizon. Furthermore, the researchers also reported that the system performed consistently across different patient groups, including sex, race, ethnicity, and insurance status.
That point matters because the study notes that demographic and clinical disparities can delay ADHD detection.
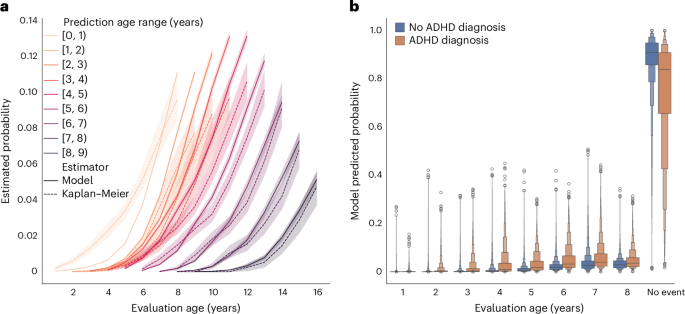
The researchers are careful about what the tool can and cannot do.
It does not diagnose ADHD.
Instead, it estimates which children may face a higher future risk. These children could benefit from earlier attention from a pediatric primary care provider or a referral to a specialist for assessment. In other words, it is meant to help direct limited time and resources, not replace clinical judgment.
“This is not an AI doctor,” said Matthew Engelhard, M.D., Ph.D., of Duke’s Department of Biostatistics & Bioinformatics and the study’s senior author. “It’s a tool to help clinicians focus their time and resources, so kids who need help don’t fall through the cracks or wait years for answers.”
That distinction runs through the study. The model works from data already collected during regular health care visits, which makes the idea appealing from a practical standpoint. No new test is described here. No new scan, blood draw, or special device appears in the report. The value comes from finding usable signals inside information that health systems already have.
The feature importance analysis added another layer to that picture. According to the study, ADHD was strongly associated with developmental, behavioral, and psychiatric conditions. That does not turn those conditions into a diagnosis on their own. However, it does suggest the model keyed in on recurring warning signs that appeared in the records before ADHD was formally recognized.
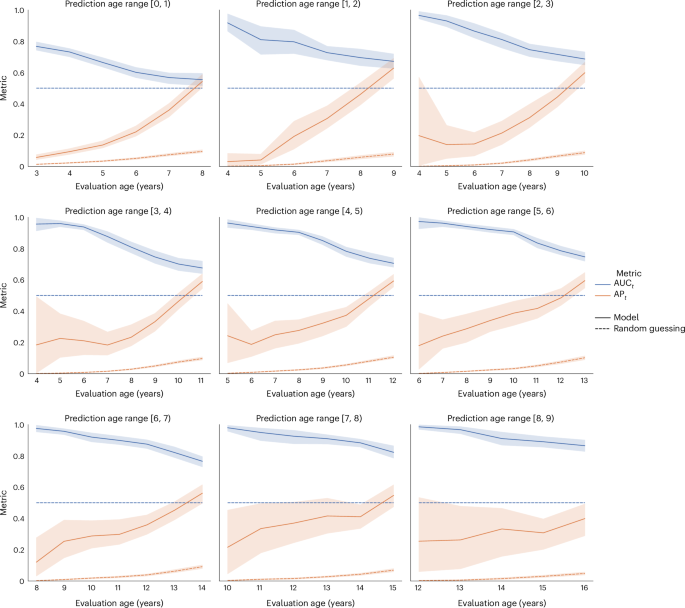
The case for earlier identification is straightforward. The researchers say earlier screening could open the door to earlier diagnosis, and in turn to earlier support. That matters because timely support is linked to better academic, social, and health outcomes for children with ADHD.
“Children with ADHD can really struggle when their needs aren’t understood and adequate supports are not in place,” said study author Naomi Davis, Ph.D., associate professor in the Department of Psychiatry and Behavioral Sciences. “Connecting families with timely, evidence-based interventions is essential for helping them achieve their goals and laying a foundation for future success.”
ADHD is described in the study as a common neurodevelopmental condition that can hurt long-term outcomes. That makes delays costly, especially when early signs are present but no diagnosis arrives for years. A system that helps flag risk earlier could give doctors and families a better chance to respond before those struggles deepen.
The study also suggests that routine electronic records may hold more predictive value than many people assume. For instance, a doctor’s visit for one issue can still leave behind details that matter later. Over time, those details may form patterns too subtle for a person to track consistently across thousands of patients. However, they are not too subtle for a trained model.
Hill and Engelhard have also studied how AI models might predict potential risks and causes of mental illness in adolescents. Therefore, this places the ADHD work inside a broader line of research on mental health prediction.
The immediate implication is not that pediatric clinics should hand diagnosis over to software. The study does not say that. In fact, the researchers stress that further studies are needed before tools like this move into clinical use.
Still, the findings suggest a plausible new role for AI in child health care. A model built from routine records could serve as an early warning system. Therefore, it may help primary care providers decide which children need more careful monitoring or earlier specialist evaluation.
That could be especially useful in cases where ADHD signs build gradually or are easy to miss during brief appointments. In addition, it could also help clinicians act sooner using information they already collect, rather than waiting until problems become more severe or more visible.
Research findings are available online in the journal Nature Mental Health.
The original story “AI scan of medical records can spot ADHD risk in children years earlier” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post AI scan of medical records can spot ADHD risk in children years earlier appeared first on The Brighter Side of News.
Leave a comment
You must be logged in to post a comment.