For over thirty years, researchers have primarily studied the accumulation of amyloid beta proteins in the brains of Alzheimer’s patients. They also focus on how that component negatively impacts neurons.
Recently, however, many researchers have become increasingly aware of the possibility that another peptide has also been overlooked as a player in this progression of neurodegeneration. Neurodegeneration is the term used to describe the effects of Alzheimer’s. This smaller peptide is derived from the same precursor as amyloid beta (Aβ). However, it is much less well known.
The hypotheses being tested, as presented in a commentary published in ChemBioChem, suggest that the peptide, which is termed P3, is not simply an innocent bystander in relation to the Aβ peptide. There is still much research to be conducted on how these peptides may affect the same pathways. These pathways can lead to neurodegeneration.
“It is likely that the P3 peptide is not the innocent bystander it has typically been considered,” stated Dr. Jevgenij Raskatov, a biochemist at the University of California, Santa Cruz. “Although more studies are needed, this could generate new approaches to treat or prevent neurodegeneration caused by Alzheimer’s.”
Progress has been slow, due in large part to investigative efforts focusing on amyloid beta as the main source of cognitive decline. As the most prevalent form of neurodegeneration in the world, Alzheimer’s has an impact on approximately 35 million individuals worldwide. It carries a total cost of nearly $800 billion annually.
Estimates predict that the total number of people with Alzheimer’s will approximately double by 2050. With nearly 400 clinical trials completed, the majority of these trials have failed to produce meaningful results. Some have only produced meaningful results with an abundance of serious side effects, such as hemorrhagic events and stroke.
Medications currently available for the treatment of Alzheimer’s disease include the use of both cholinesterase inhibitors and NMDA receptor antagonists. These produce only temporary symptomatic relief and do not change the course of the disease.
Additionally, as of the past year, a new class of antibody medications is being developed to reduce levels of amyloid beta from the brain, such as lecanemab and donanemab. These treatments are expected to have limited outcomes. “The current state of Alzheimer’s therapies is extremely slow-moving and leaves much room for improvement,” added Raskatov. “We are in dire need of completely new approaches.”

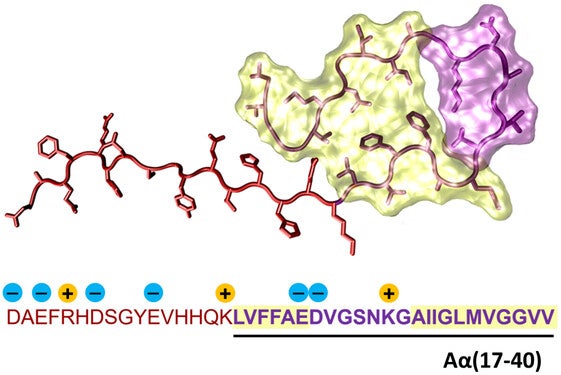
A P3 peptide has recently caught the interest of researchers due to its unique characteristics. It has been on the radar of scientists since they first identified that it originated from a different enzymatic pathway than amyloid β through digestion. They also found that it has an aggregation potential that exceeds that of amyloid β. The fact that P3 originates from a different source than amyloid β and is produced by enzymes is of great interest to Raskatov et al.
The P3 peptide has been known to be produced through different enzymatic pathways. While the enzymes responsible for producing P3 were assumed to be harmless and to produce only water-soluble peptides, extensive research done within the last five years has demonstrated that the P3 peptide is indeed capable of forming microscopic aggregates and fibrils. It may also produce them much more quickly than amyloid β. In addition, P3 appears to interact directly with amyloid β, causing it to accumulate and become more toxic to neurons.
Some of the initial findings of the Raskatov group show that the P3 peptide can cause neuronal damage, although it is reported to be less toxic than amyloid β. There are also still many unanswered questions regarding the biological roles of P3.
The researcher Raskatov has shown how P3 may also be toxic and has linked the toxicity to a pathway for generating aggregated forms of aggregation-prone proteins. Whether generated from mixed aggregates or not, the aggregation of two or more aggregation-prone protein forms may be responsible for producing toxic oligomers. This process may contribute to neurotoxicity associated with age-dependent diseases.
As more research continues to be published about Alzheimer’s disease, new insights are expected to dramatically improve both the clinical practice of diagnosis and the development of novel therapies.
These advances may also improve the understanding of what constitutes an effective treatment for Alzheimer’s disease.
Research findings are available online in the journal ChemBioChem.
The original story “A lesser-known brain peptide may contribute to Alzheimer’s disease” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post A lesser-known brain peptide may contribute to Alzheimer’s disease appeared first on The Brighter Side of News.