As men get older, changes in sexual health and fertility are often expected. For decades, the usual explanation has been a drop in testosterone or simply the aging process itself. But new research challenges that idea and offers a hopeful outlook. A large study, recently presented at ENDO 2025 in San Francisco, points to something much more manageable—blood sugar.
According to researchers, even a small increase in blood sugar can quietly shape the way a man’s body handles sex and reproduction. That change can happen long before diabetes sets in. The good news is that this shift can be slowed or even reversed. And it doesn’t require drastic measures—just better daily habits and early health checkups.
From 2014 to 2020, scientists tracked the health of 200 men, aged 18 to 85, who had no major health issues such as diabetes, heart disease, or cancer. By the end, 117 men remained in the study. Their health was examined across multiple areas, including hormone levels, sperm quality, blood sugar, body mass index (BMI), and sexual functioning.

Participants were selected because they represented healthy individuals. This helped researchers understand how aging alone, without other health complications, affects sexual and reproductive systems. The research was led by Dr. Michael Zitzmann, a medical doctor and professor at University Hospital in Muenster, Germany.
Throughout the six-year period, the men underwent regular tests for semen quality, hormone levels, and metabolic markers. One key marker was HbA1c, a test that shows average blood sugar over the past few months. Even when levels stayed below the 6.5% threshold used to diagnose diabetes, small rises in blood sugar were linked to changes in sexual health. What they found was both surprising and promising.
Despite the natural aging process, hormone levels and semen profiles largely stayed within normal limits. That means men continued to produce healthy amounts of sperm and maintained typical hormone ranges, including testosterone.
However, two areas showed a steady decline in those with slightly raised blood sugar: sperm motility and erectile function. Sperm motility refers to how well sperm can move, which is crucial for fertility. Erectile function, on the other hand, plays a major role in sexual satisfaction and overall quality of life.
“These changes more closely correlate with modest increases in blood sugar and other metabolic changes,” Dr. Zitzmann explained. “Although age and testosterone levels have long been considered an impetus for men’s declining sexual health, our research indicates otherwise.”
He also pointed out that testosterone did not seem to affect erectile function directly. Instead, it was more connected to libido, or sexual desire. This distinction could help doctors offer more personalized treatment strategies. Instead of focusing only on testosterone levels, they might now screen and manage early signs of blood sugar imbalance.
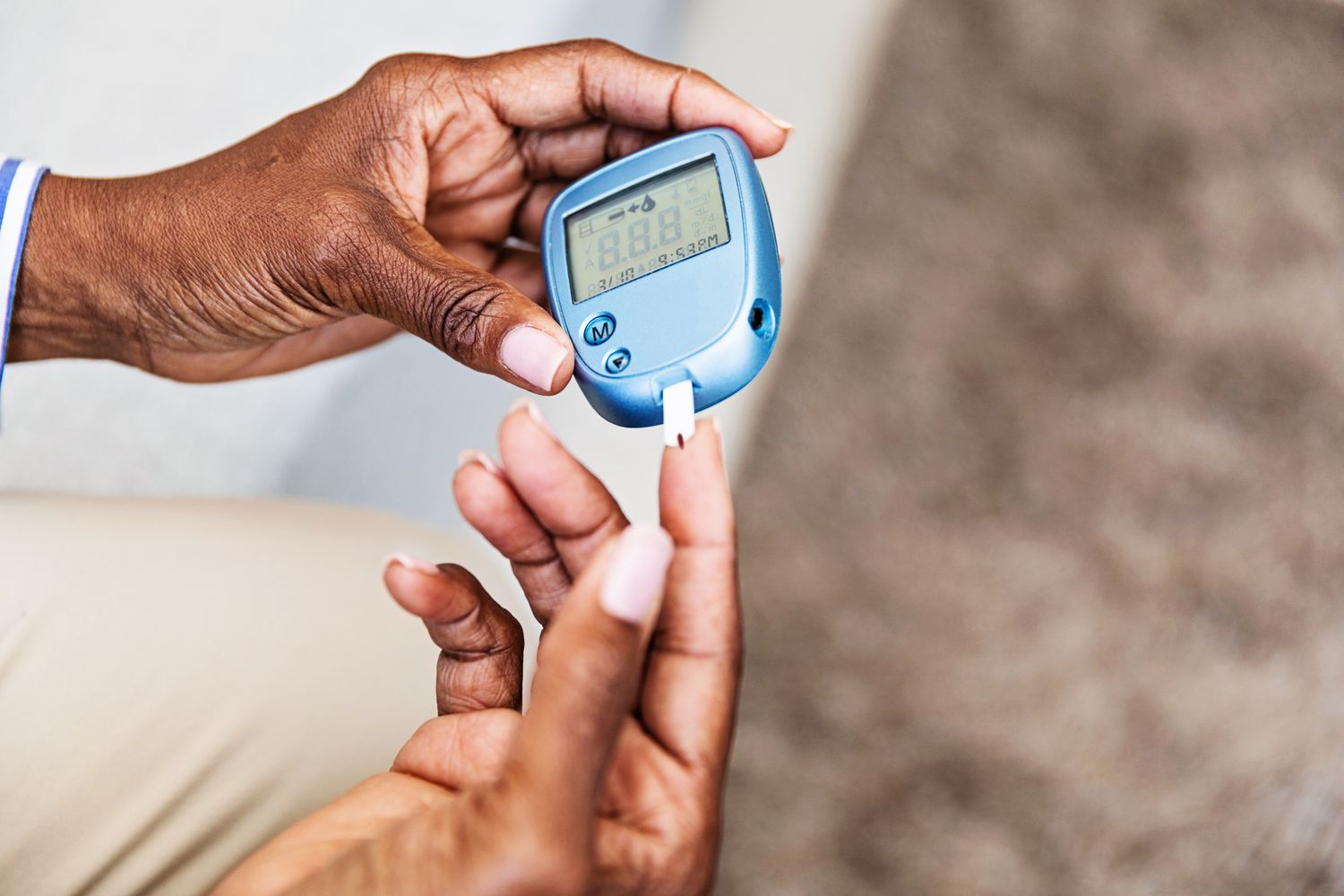
Blood sugar levels can begin to rise quietly, especially as metabolism slows with age. People often don’t notice until much later when symptoms become obvious or a diagnosis like Type 2 diabetes is made.
This new data offers a different path forward. By catching small changes early—before they cross into diabetic territory—men can take action. Healthier eating, regular physical activity, better sleep, and stress management can all help keep blood sugar stable.
Medical options also exist for those who need more help. But most importantly, the study suggests that men have far more control over their sexual and reproductive health than previously believed. “We now know that it’s in our power to retain sexual and reproductive wellbeing in men, even as they age,” said Dr. Zitzmann. “This means that men can take steps to preserve or revive their reproductive health with lifestyle choices and appropriate medical interventions.”

This study could lead to changes in how doctors talk to and treat their male patients. Rather than blaming all symptoms on age or testosterone, providers may start looking at small but important metabolic clues. The hope is that doctors can create new health plans with their patients that focus on prevention. For example, they might include routine HbA1c testing for men in their 30s, 40s, and beyond—even if they show no signs of illness.
Patients can also be encouraged to ask about these options. Catching early blood sugar shifts not only helps prevent diabetes but may also protect against frustrating sexual health issues that are often kept quiet. By linking blood sugar to reproductive function, this study opens up a fresh way to think about men’s health.
It’s not just about aging gracefully—it’s about being proactive with simple steps that really make a difference.
Note: The article above provided above by The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post Blood sugar is key to men’s reproductive health, study finds appeared first on The Brighter Side of News.