Minutes matter when a surgeon is deciding how much tissue to remove. Yet for centuries, medical imaging has leaned on stains and dyes that take time and change what you are trying to study. During surgery, traditional staining can take 20 to 30 minutes, and that pause can slow decisions about tumor margins. In routine pathology, the wait often stretches longer because samples go through preparation steps that alter the very molecules under inspection.
A new handheld device aims to change that rhythm. In a paper, researchers led by Professor Guoan Zheng at the University of Connecticut describe a deep-ultraviolet ptychographic pocket-scope called DART. The name is short, but the idea is sweeping. Instead of relying on dye binding, the device reads signals that already exist inside living material.
“DART provides molecular information instantly, and because it’s based on intrinsic molecular properties rather than dye binding, the results are inherently quantitative and reproducible,” Zheng said.
The system uses deep-ultraviolet light to measure how DNA and proteins naturally absorb specific wavelengths. That absorption becomes a direct, built-in contrast method. With it, DART can create quantitative maps of key molecules with femtogram precision, without adding labels, and without waiting for stains to develop.
Stains have a long history for a reason. Without them, many tissues look pale and hard to read. Dyes make the nucleus stand out. They highlight proteins. They give clinicians familiar patterns that guide diagnosis.
But staining also creates tradeoffs. It can delay care during time-sensitive moments. It can require chemicals, equipment, and trained staff. It can also modify the molecules you want to measure, which complicates efforts to study biology in its natural state.
DART targets that exact pain point. The approach starts with a simple observation: DNA and proteins already absorb deep-ultraviolet light in distinct ways. If you shine the right wavelengths through tissue and capture what gets absorbed, you can map those molecules directly.
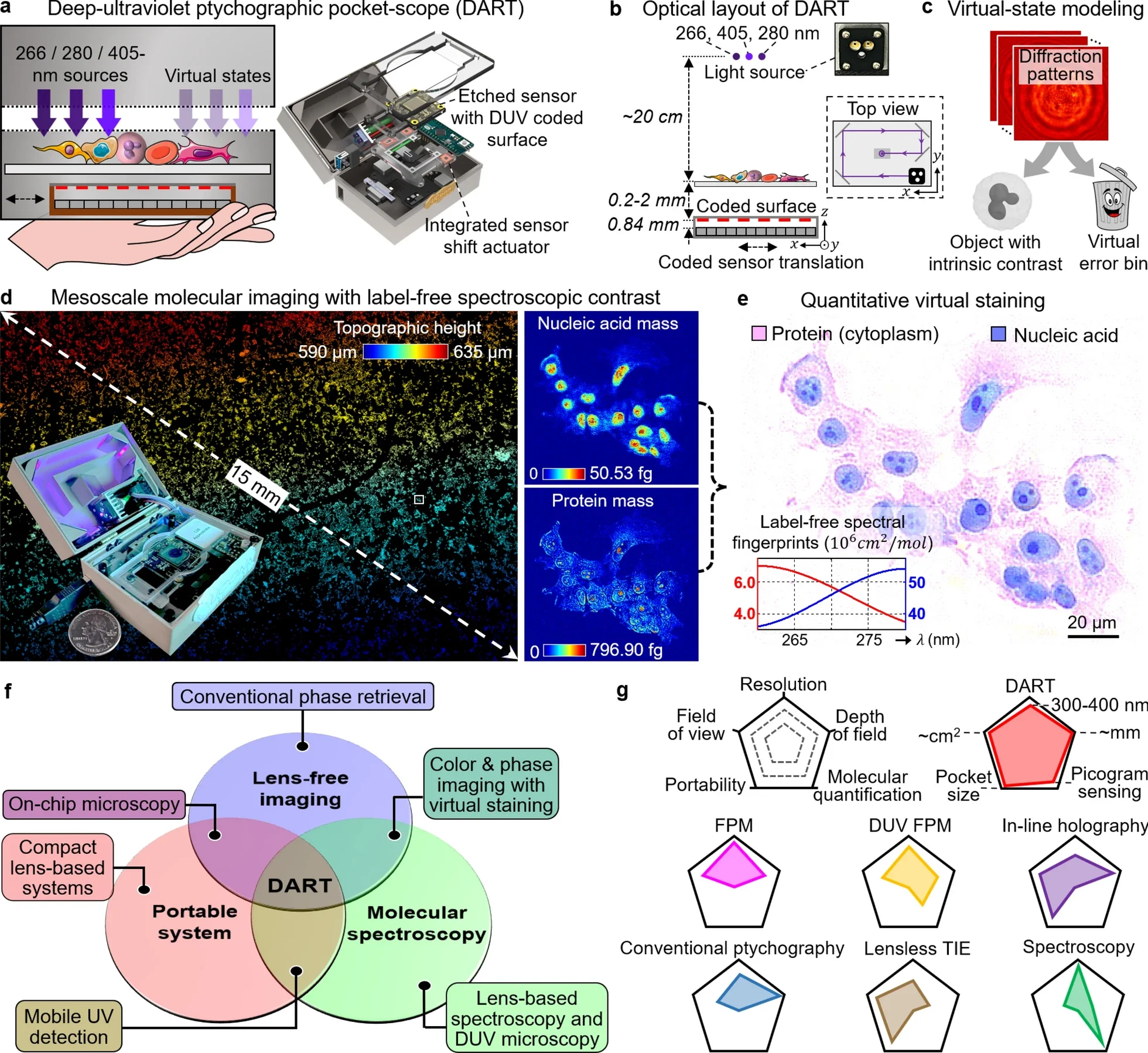
The research team focused on 266 and 280 nanometers. At these wavelengths, nucleic acids and proteins show different absorption signatures. DART measures that difference and turns it into a quantitative picture, not just a pretty image.
DART is not built like a standard microscope. Traditional microscopy often depends on lenses and labeling. This platform leans on computational imaging, deep-ultraviolet spectroscopy, and a pocket-sized design.
By imaging at 266 and 280 nanometers, the device separates nucleic-acid-rich regions from protein-rich regions. It then builds molecular maps that quantify mass with femtogram accuracy. You get a picture that is grounded in measured molecular content, not guesswork.

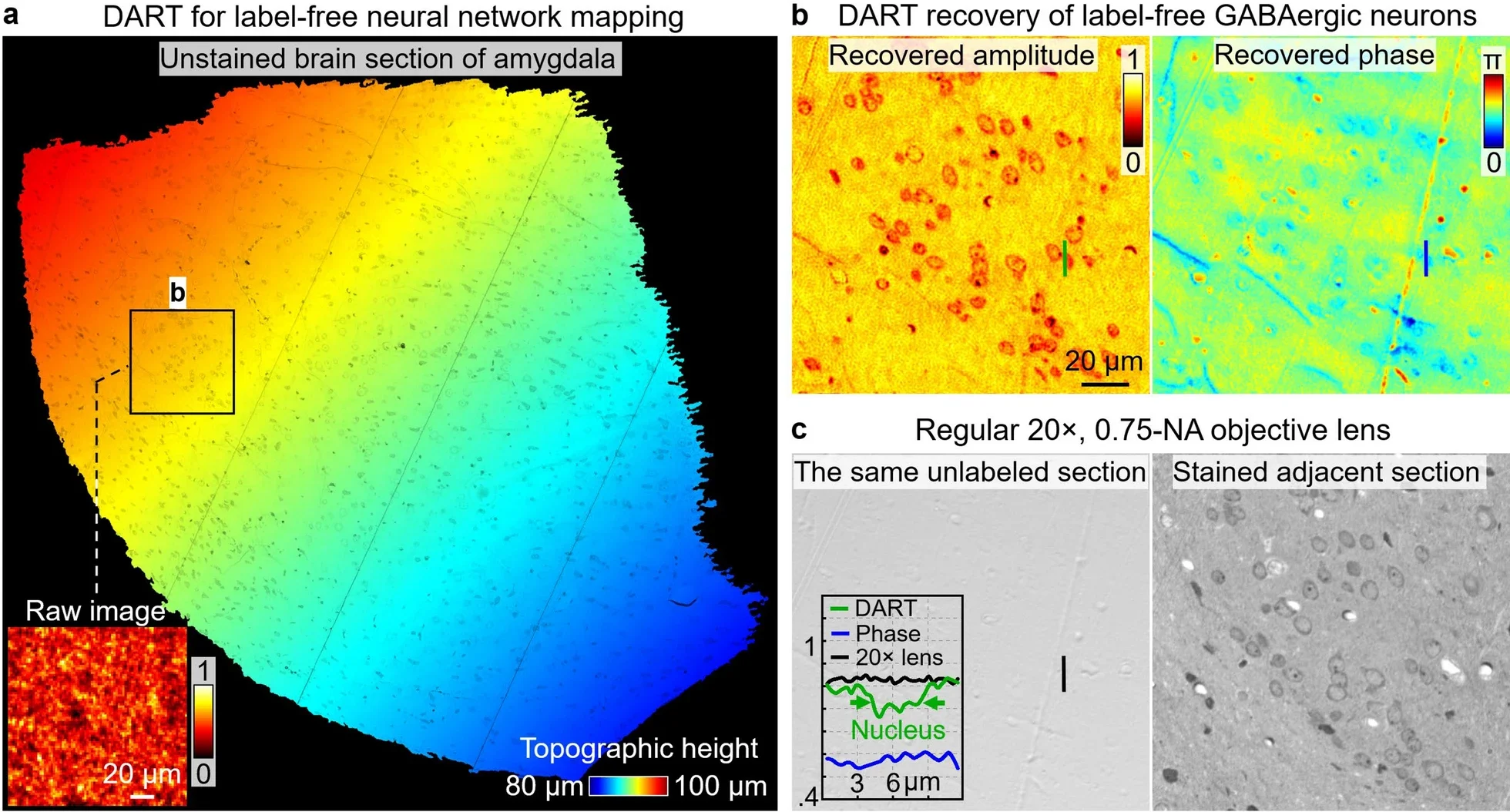
This is where the system’s “virtual staining” matters. You still want an image that looks like what pathologists know how to read. DART translates measured DNA and protein distributions into familiar histology-style appearances, but it does so using actual data from the sample.
The team draws a sharp contrast with AI-only virtual staining methods, which can introduce artifacts or hallucinated features. DART’s virtual stains derive from measured molecular content, not from a model’s best guess.
“We’re essentially giving clinicians molecular X-ray vision,” Zheng said. “hey can see not just cell structures, but the actual protein and DNA distributions that define cellular identity and pathological states.”
The device’s performance targets a frustrating limitation in conventional microscopy: you usually trade field of view for detail, and you often trade depth of field for sharpness. DART is designed to hold several advantages at once.
The system reaches 308-nanometer resolution in a handheld form. It offers a centimeter-scale field of view and a millimeter-scale depth of field. That combination lets you capture broad tissue regions without constant mechanical refocusing.
In practical terms, it means you can scan larger areas quickly while still seeing fine structure. You can also keep more of the sample in focus at once. For tissue assessment, that wide view can matter as much as raw resolution.
The approach also aims for reproducibility. Because the contrast comes from intrinsic absorption, the measurement does not depend on how evenly a dye penetrates or how long the stain sat. That consistency becomes especially valuable when clinicians compare samples over time, or when researchers compare results across labs.
To make deep-ultraviolet imaging work in a pocket device, the team had to solve several technical problems. Deep ultraviolet light is demanding. Many commercial sensors are not built to capture it well. Optical systems can also struggle when light coherence is limited, especially with LEDs.
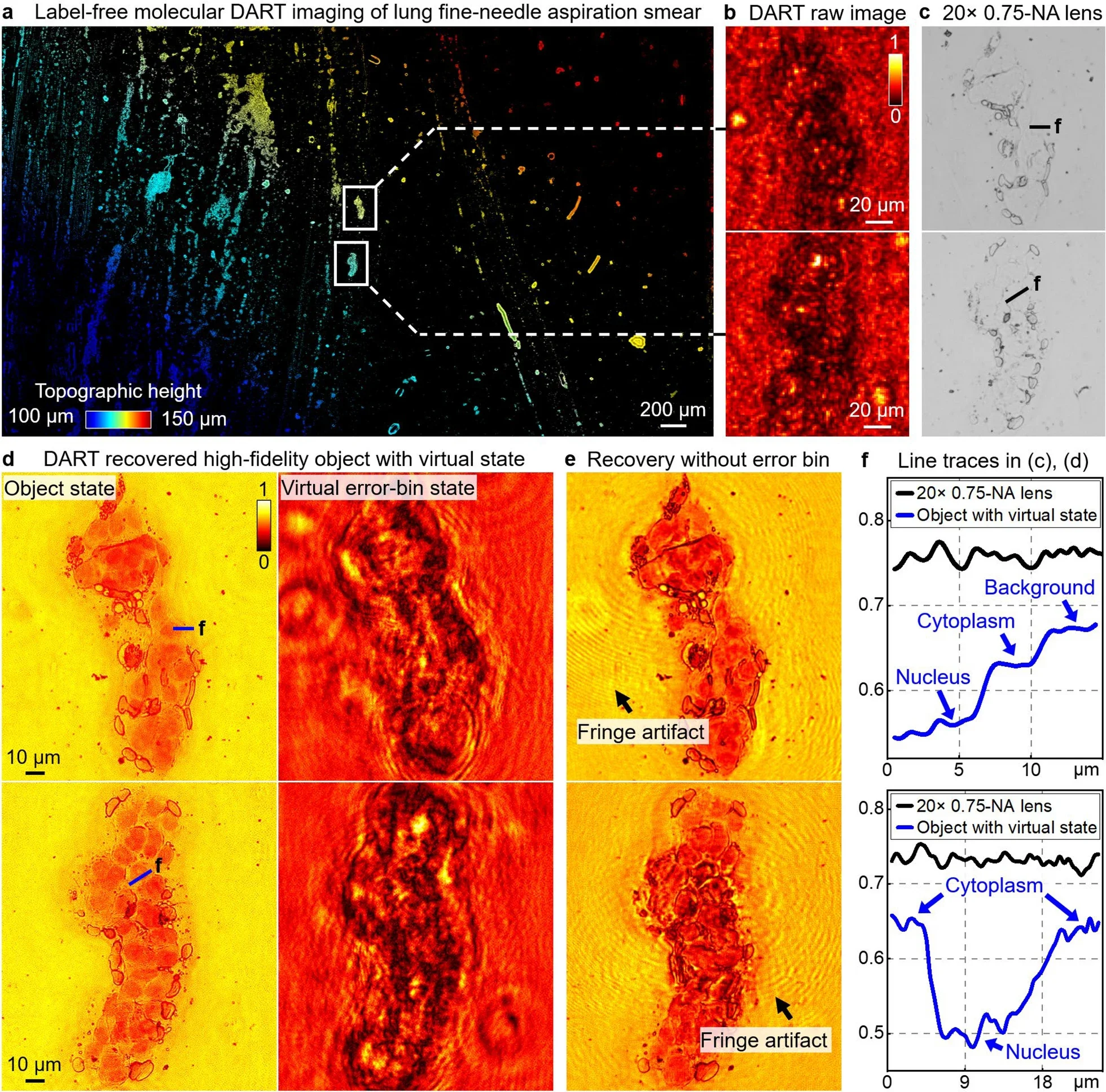
The researchers report several innovations to overcome these barriers. They modified commercial image sensors to improve deep-ultraviolet sensitivity. They also used a disorder-engineered coded surface that converts high-angle scattered light into signals the sensor can detect.
A key step involves their “virtual state” algorithm. The method is designed to reduce artifacts linked to LED coherence limitations and optical imperfections. That matters because small errors can create misleading structures in imaging. The goal here is clarity without false detail.
The research team frames DART as more than a faster microscope. It is a workflow shift. If a clinician can get molecular information instantly, they may spend less time waiting for stains and more time acting on results.
The study points toward real-time surgical guidance as an obvious use case. When a surgeon needs to assess margins, speed and reliability matter. A handheld platform that avoids staining could fit into that setting more naturally than a lab-heavy approach.
The design also points to field diagnostics. Many settings lack staining infrastructure. Some clinics do not have staff, reagents, or time for standard protocols. A compact, label-free system could bring advanced imaging closer to where patients actually are.
The team also highlights space missions. In microgravity, monitoring astronaut health and tracking microbial adaptation can become urgent, yet laboratory tools must be compact and reliable. A handheld, label-free platform could support that work because it reduces dependencies on consumables and complex prep.
Looking ahead, the researchers describe plans to expand the wavelength range to improve molecular discrimination. They also envision endoscopic versions for in vivo imaging, which could push the technology closer to direct use inside the body.
DART could speed decisions in settings where time is tight, especially during surgery. If clinicians can view tissue without waiting for dyes, they may shorten pauses that delay treatment choices. The approach also keeps samples closer to their natural state, which may help reduce confusion caused by preparation steps that alter molecules.
For pathology and research, the biggest shift is quantitative, label-free measurement. By mapping DNA and protein content directly, DART may support more consistent comparisons between samples and across institutions. That consistency can strengthen studies that rely on subtle tissue differences and can make results easier to reproduce.
The portability of the platform could also widen access. Clinics without staining resources may still be able to perform meaningful tissue assessment. In space biology, a compact tool that avoids consumables may help teams track health changes and microbial behavior during long missions.
Over time, the same core idea, measuring intrinsic molecular signatures, could open new ways to study disease while preserving the sample’s true chemistry.
Research findings are available online in the journal eLight.
The original story “New deep-UV pocket scope provides instant molecular imaging” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post New deep-UV pocket scope provides instant molecular imaging appeared first on The Brighter Side of News.
Leave a comment
You must be logged in to post a comment.