A cloud of fruit scent or mint can hide what matters most: what happens after the aerosol hits living tissue.
That question sits at the center of a new review led by UNSW Sydney, which argues that nicotine-based e-cigarettes are likely to cause cancers of the lung and oral cavity. Published in Carcinogenesis, the paper pulls together clinical findings, animal experiments and laboratory research to ask a narrower question than many earlier debates about vaping. Not whether vaping is better than smoking, but whether it may cause cancer in its own right.
“To our knowledge, this review is the most definitive determination that those who vape are at increased risk of cancer compared to those who don’t,” said Adjunct Professor Bernard Stewart AM, the UNSW cancer researcher who led the study.
The review includes investigators from The University of Queensland, Flinders University, The University of Sydney, Royal North Shore Hospital, The Prince Charles Hospital and Sunshine Coast University Hospital. The group included pharmacists, epidemiologists, thoracic surgeons and public health researchers.
Their conclusion is blunt. “Considering all the findings, from clinical monitoring, animal studies and mechanistic data, e-cigarettes are likely to cause lung cancer and oral cancer,” Stewart said.
For years, much of the public-health discussion around e-cigarettes focused on whether they help smokers quit or steer young people toward tobacco. The new review says that framing left a major question underexplored: whether vaping itself may be carcinogenic, even in people whose risk cannot be blamed on cigarette smoke.
That distinction matters because the authors deliberately excluded findings from dual users, people who both smoke and vape, from the core assessment of vaping’s independent cancer risk. In those cases, tobacco smoke can muddy the picture.
The devices themselves have changed quickly since the early 2000s, from early electronic cigarettes to pod systems and disposables. Yet their basic setup remains similar: a battery, a heating coil and an e-liquid, usually containing nicotine and flavorings, that becomes an inhaled aerosol.
The review focused only on nicotine-delivering e-cigarettes, not products used for cannabis or other drugs.
Long-term population studies that track cancer rates in exclusive vapers still do not exist. Lung cancer can take decades to emerge, and e-cigarettes have not been around long enough for that kind of evidence to fully mature.
So the researchers leaned on other kinds of evidence already used in cancer research. They examined biomarkers in people who vape, including signs of DNA damage, oxidative stress, inflammation and epigenetic change. They also looked at tissue injury in the lungs and mouth.
Across those studies, the pattern was hard to ignore.
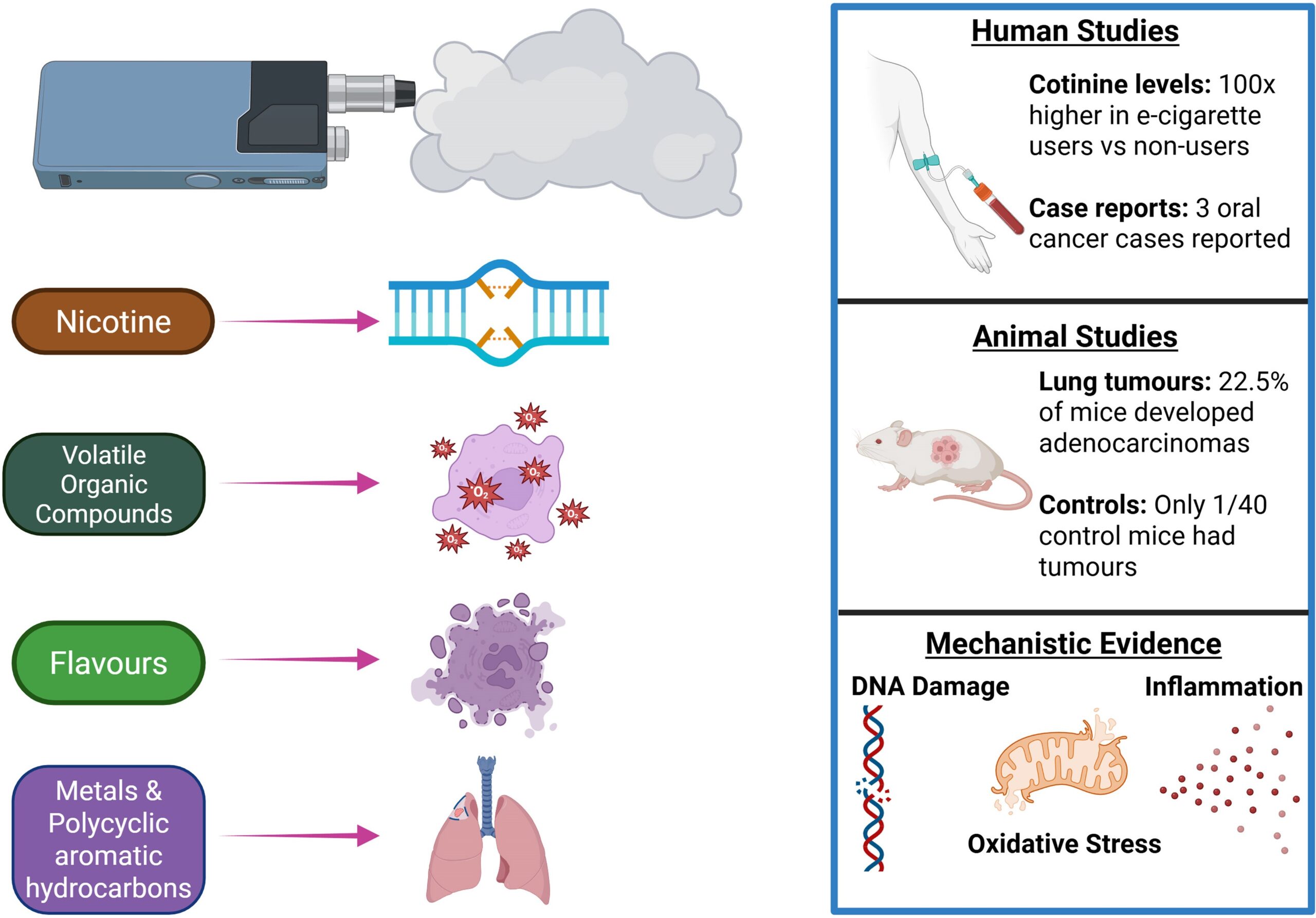
The review points to numerous carcinogenic compounds in e-cigarette aerosols, including volatile organic chemicals and metals released from heating elements. Urine and blood studies found evidence that users absorb and process substances such as nicotine metabolites, tobacco-specific nitrosamine markers, certain volatile organic compounds and metals.
Some reported differences were large. One review cited in the paper found urinary cotinine levels in e-cigarette users were more than 100 times higher than in nonusers. Another 2025 study of 3,353 exclusive e-cigarette users found nicotine e-cigarette users had mean concentrations of total nicotine equivalents and cotinine at least 100-fold higher than users of non-nicotine e-cigarettes.
Human studies of oral cells also found higher levels of DNA adducts and other markers linked to genetic injury. Reviews summarized in the paper described increased oxidative stress in e-cigarette users compared with nonsmokers, as well as inflammatory changes and altered methylation patterns associated with cancer-related pathways.
On the oral side, the review notes changes to the microbiome, inflammation and tissue damage that some earlier studies linked to oral cancer risk.
One of the most striking findings in the review comes from an animal study by Tang and colleagues. Mice exposed to e-cigarette aerosol for 54 weeks developed lung tumors at a far higher rate than control animals.
Nine of 40 aerosol-exposed mice, or 22.5%, developed lung adenocarcinomas. Among 40 controls, one mouse developed a lung tumor. The same experiment also found hyperplastic bladder changes in 23 of 40 aerosol-exposed mice, though the new review stops short of making bladder cancer its main conclusion.
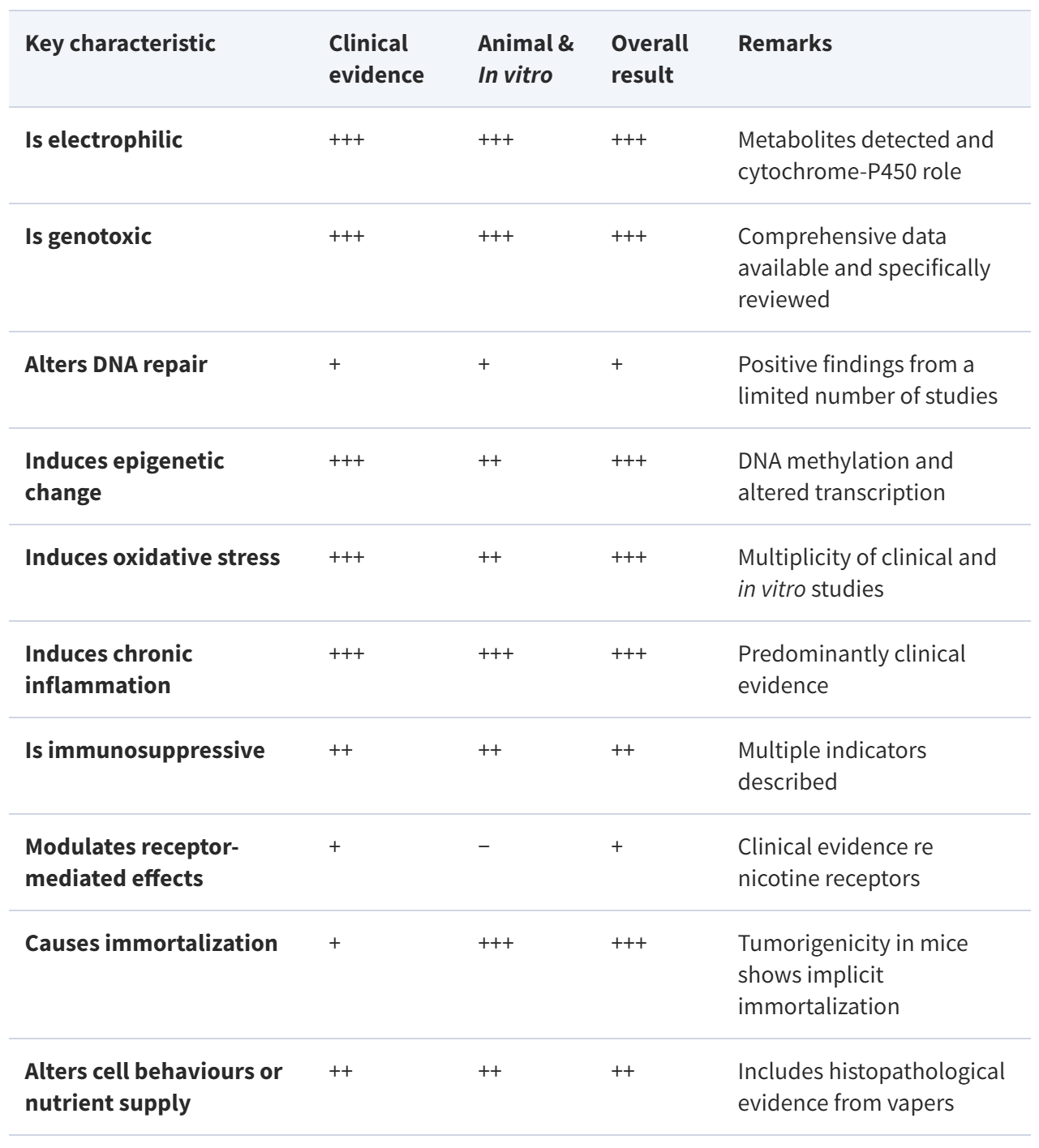
Laboratory evidence added another layer. The authors say e-cigarette aerosols, taken as a mixture, implicate all 10 of the “key characteristics of carcinogens,” a framework used to organize mechanistic cancer evidence. The review describes support for genotoxicity, oxidative stress, chronic inflammation, epigenetic change, immune disruption and altered cell behavior, among other traits associated with carcinogens.
That breadth matters because it suggests vaping is not acting through one simple pathway. It looks more like a complex chemical exposure with multiple ways of damaging tissue.
The paper also points to carcinogenic substances already known from other settings, including benzene, formaldehyde, acrylamide, nickel and chromium-related compounds, alongside nicotine-derived nitrosamine processes that may have their own carcinogenic role.
The authors are careful about what they are not claiming.
“Our assessment is qualitative and does not involve a numerical estimate of cancer risk or burden,” Stewart said. “We’ll only be able to determine the precise risk once longer-term studies are available.”
That limitation runs through the paper. There are no large epidemiological studies yet comparing cancer incidence in exclusive e-cigarette users and nonusers. Some human biomarker studies are small. Different studies also use different devices, exposure measures and biological markers, which makes meta-analysis difficult.
Case reports exist, including reports of oral cancers in longtime e-cigarette users and one lung cancer case involving a man with both e-cigarette use and a past smoking history. But case reports cannot prove causation on their own.
Even so, the authors argue that the consistency across evidence streams, clinical, animal and mechanistic, now supports a firm public-health warning.
Associate Professor Freddy Sitas of UNSW put it plainly: “The evidence was remarkably consistent across fields. It dictated an unequivocal finding now, though human studies that estimate the risk will take decades to accumulate.”
He also warned that vaping rarely stays confined to vaping. “Most of those who use e-cigarettes to quit smoking end up in ‘dual-use-limbo’, unable to shake off either habit,” he said.
The paper notes recent U.S. epidemiological evidence showing that people who both smoke and vape face an additional four-fold increased risk of developing lung cancer.
Sitas and Stewart also draw a historical parallel. Smoking was not officially recognized as a cause of lung cancer until 1964, despite warning signs that had surfaced much earlier.
“E-cigarettes were introduced about 20 years ago. We should not wait another 80 years to decide what to do,” Sitas said.
That line captures the paper’s larger argument. Waiting for perfect long-term proof can become its own form of public-health failure.
This review does not calculate exactly how many cancers vaping may cause. It does something more immediate. It argues that the available evidence is already strong enough to treat nicotine-based e-cigarettes as a likely cancer risk, not merely a cleaner-looking substitute for cigarettes.
For regulators, that supports tighter control of availability and stronger public warnings. Meanwhile, for clinicians, it suggests vaping should be discussed not only in terms of addiction or quitting, but also possible cancer risk.
For the public, especially younger users, the message is that the absence of decades-long data is not the same as the absence of danger.
Research findings are available online in the journal Carcinogenesis.
The original story “Study finds surprising new link between vaping and cancer” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post Study finds surprising new link between vaping and cancer appeared first on The Brighter Side of News.
Leave a comment
You must be logged in to post a comment.