Feelings like hopelessness and loss of pleasure may leave traces in the immune system that standard depression screening cannot yet see.
A new study of 440 women found that a blood-based measure of aging in monocytes, a type of white blood cell tied to immune defense, tracked with the cognitive and emotional symptoms of depression more than with physical complaints such as fatigue or appetite changes. The work points to a possible biological marker for certain forms of depression, especially in women living with HIV, who face a higher burden of the disorder.
That matters because depression still has no lab test.
Doctors diagnose it through reported symptoms and by ruling out other conditions. Yet depression is not one illness with one pattern. Some people feel slowed down, agitated, tired, or unable to sleep. Others mainly struggle with loss of pleasure, hopelessness, guilt, or the sense that they have failed. Those differences can make the condition harder to catch, especially when physical symptoms overlap with chronic disease.
“Depression is not a one-size-fits-all disorder, it can look really different from person to person, which is why it’s so important to consider varied presentations and not just a clinical label,” said Nicole Beaulieu Perez, an assistant professor at NYU Rory Meyers College of Nursing and the study’s author. “Our study reveals unique biological underpinnings of mental health that are often obscured by broad diagnostic categories.”
The research, published in The Journals of Gerontology Series A, drew on data from the Women’s Interagency HIV Study. The sample included 261 women with HIV and 179 without HIV. Depression symptoms were measured with the 20-item Center for Epidemiologic Studies Depression Scale, known as the CES-D.
The women were, on average, 42 years old. About 35% identified as Black and 48% as Hispanic.
Rather than treating depression as a single number, the team broke symptoms into somatic and non-somatic categories. Somatic symptoms included bodily complaints such as sleep, appetite, and concentration problems. Non-somatic symptoms covered affective, cognitive, and interpersonal experiences, including anhedonia, hopelessness, and feelings of failure.
The researchers then compared those symptom patterns with measures of biological aging from blood samples. They used two epigenetic clocks, tools that estimate biological age from chemical marks on DNA. One was the Horvath clock, a broad multi-tissue measure. The other, called MonoDNAmAge, focused specifically on monocytes.
That choice was central to the study.
Monocytes sit at the crossroads of aging, inflammation, and HIV. They play an important role in immune responses, are involved in HIV infection and progression, and have been linked in earlier work to depression. By using a clock built from monocyte DNA methylation rather than from mixed cell types, the team hoped to capture a more specific biological signal.
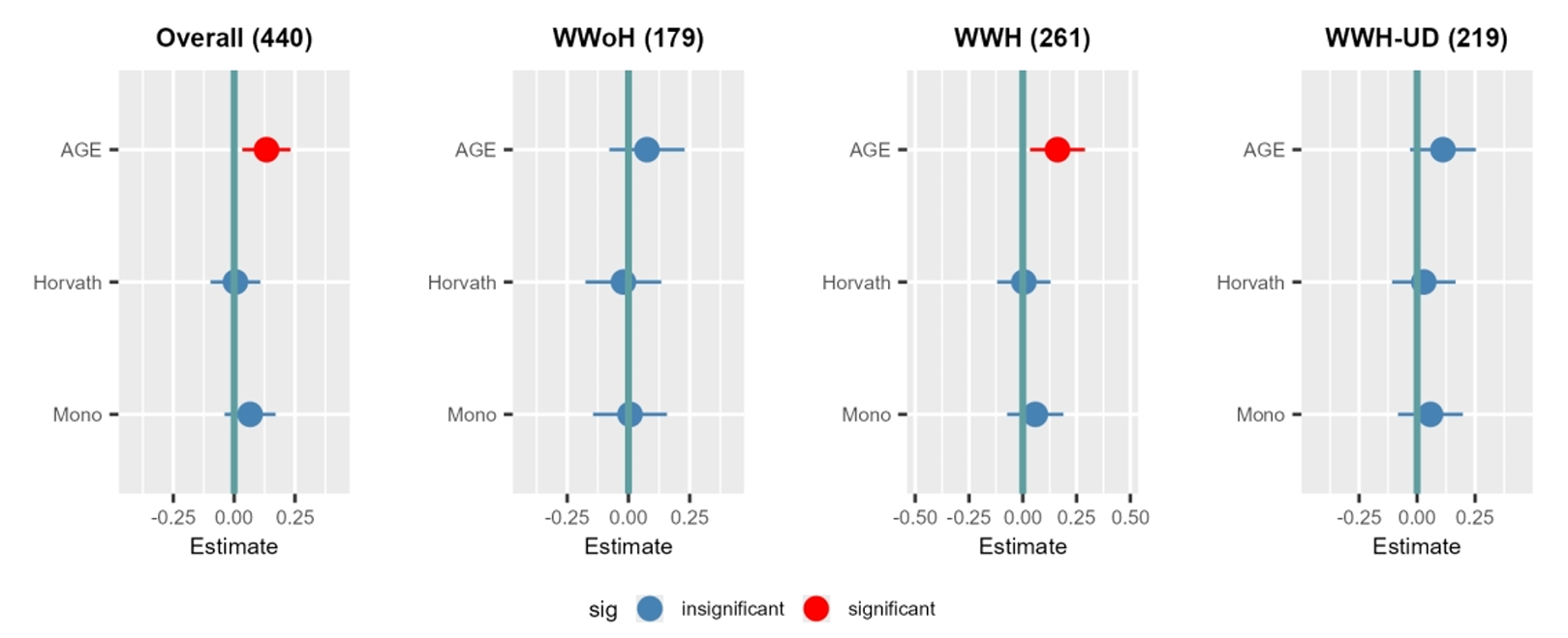
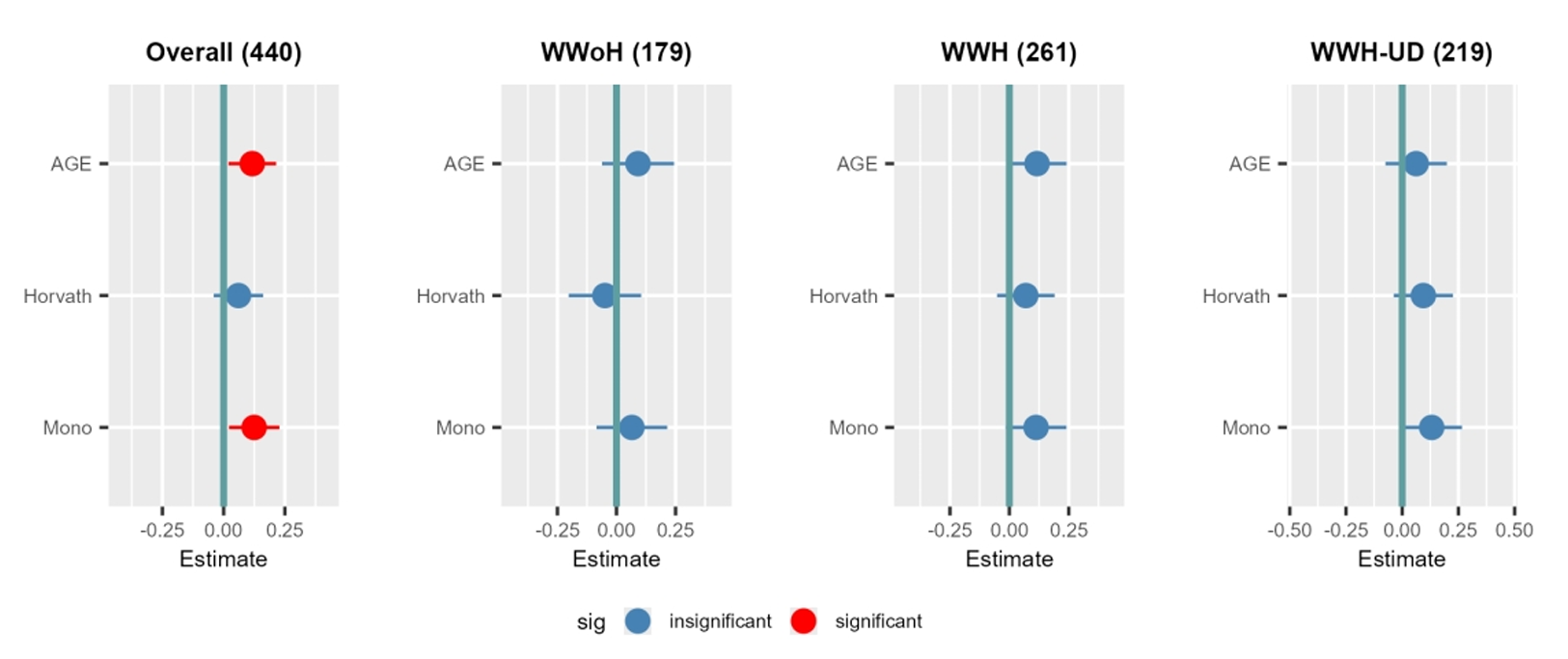
In the full sample, faster monocyte aging was significantly associated with higher total depression scores. But the sharper pattern appeared when the symptoms were split apart.
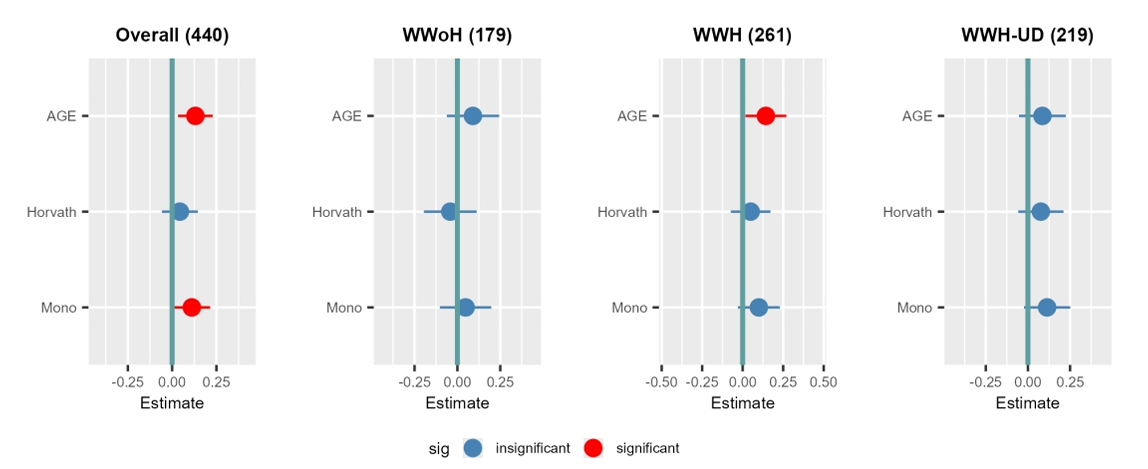
Monocyte age acceleration was tied to the non-somatic side of depression, not the somatic side. In the overall group, it was significantly associated with non-somatic symptoms, while neither the monocyte clock nor the Horvath clock showed an association with somatic symptoms.
At the item level, the monocyte measure lined up most clearly with anhedonia, hopelessness, and feelings of failure. It was also associated with sleep disturbance in the overall sample. Among women with HIV, the pattern looked broadly similar, though some findings in smaller subgroup analyses did not meet the study’s cutoff for statistical significance.
The Horvath clock told a different story. It was not associated with total depression scores or with the broader symptom domains. Instead, it showed links to a few individual items in the overall sample, including inability to shake “the blues,” crying, and sleep disturbance.
That contrast suggests different biological aging measures may be sensitive to different parts of what gets lumped together as depression.
“This is particularly interesting because people with HIV often have physical symptoms like fatigue that are attributed to their chronic illness rather than a depression diagnosis. But this flips that on its head because we found that these measures are associated with mood and cognitive symptoms, not somatic symptoms,” said Perez.
Depression is already known to be more common in people living with HIV, and the burden falls especially hard on women. The source material notes that depression is two to three times more common in women with HIV than in men or unaffected women, with rates ranging from 35% to 60%.
Its effects can spill into care. Depression has been linked to lower adherence to antiretroviral therapy, reduced CD4+ T cell counts, and increased viral transmission.
Perez said the goal is to catch the condition sooner. “For women with HIV who may be experiencing depression, we want to better understand what’s going on and catch it earlier so that it doesn’t harm their whole overall health.”
A majority of the women with HIV in this analysis had undetectable viral loads, which makes the findings more interesting. The relationship between monocyte aging and depressive symptoms may not be just a sign of uncontrolled infection. The authors note that even with effective treatment, people living with HIV can still face earlier onset of chronic, age-related health problems.
The results also fit with a growing idea in psychiatry that some depressive symptoms may be linked to inflammatory or immune-related pathways. In this case, the symptoms that stood out most strongly, especially anhedonia and hopelessness, matched that picture better than the physical complaints did.
The work has clear limits.
It was cross-sectional, meaning it captured one slice in time and cannot show whether accelerated monocyte aging helps cause depression, results from it, or both. The CES-D is widely used, but it does not cover every kind of depressive presentation, including some atypical features. The item-level analysis was exploratory, and the team did not apply a multiple-comparison correction.
The subgroup findings also need caution. Some associations seen in women with HIV did not reach formal statistical significance, likely in part because the smaller samples reduced power.
Even so, the analysis had strengths. It focused on a population often overlooked in biological psychiatry research, reduced some of the noise that comes from mixing different cell types together, and compared a monocyte-specific clock with a broader aging clock in the same study.
The findings do not mean a depression blood test is ready for the clinic. They do suggest that the search for one may need to move away from treating depression as a single, uniform diagnosis.
A marker that tracks hopelessness, anhedonia, or related cognitive symptoms could help clinicians notice cases that might otherwise be missed, especially in people whose physical symptoms are easily explained by another illness. Longer term, Perez said, that kind of biological readout could support more tailored care.
“I think about the adage, ‘What gets measured gets managed.’ An aspirational goal in mental health would be to combine subjective experience with objective biological testing,” she said. “Our findings bring us a step closer to this goal of precision mental health care, especially for high-risk populations, by providing a biological framework that could guide future diagnosis and treatment.”
Research findings are available online in The Journals of Gerontology Series A.
The original story “Study links biological aging to cognitive effects of depression” is published in The Brighter Side of News.
Like these kind of feel good stories? Get The Brighter Side of News’ newsletter.
The post Study links biological aging to cognitive effects of depression appeared first on The Brighter Side of News.
Leave a comment
You must be logged in to post a comment.